Air embolism, Central venous catheter, Hypovolemic shock, Septic shock, Cardiorespiratory arrest
An early 60's-year-old woman with breast cancer, undergoing chemotherapy by central venous catheter (CVC) in the right subclavian vein, had experienced abdominal pain, intractable vomiting for two days and an isolated fever spike. She enters the Emergency Room (ER) with a Glasgow Coma Scale of 7, hypotension and desaturation. Blood gas analysis revealed respiratory failure, severe anaemia (haemoglobin 4.9 mg/dL) and hyperlactacidemia. Fluid therapy, vasopressor and transfusion support were initiated. Further tests showed severe pancytopenia and signs of multiple organ disfunction (acute kidney injury, coagulopathy and hyperbilirubinemia). A computed tomography scan showed evidence of massive gas embolism in different organs and vascular structures as presented in the (Figure 1 and Figure 2). Air embolism was interpreted as a likely complication of the use of the CVC associated with a multifactorial shock (hypovolemic and septic). The shock probably increased the risk of air entry via an increased gradient between the external atmospheric pressure and the low central venous pressure [1]. She developed cardiorespiratory arrest and died despite advanced life support.
Air embolism is a potentially preventable complication, but it can have severe consequences if not recognized and treated promptly [2,3]. Treatment focuses on three key objectives: preventing further embolus progression, reducing gas volume, and evaluating the need for advanced interventions. Standard management involves administering high-concentration oxygen to accelerate gas reabsorption and positioning the patient in Durant's maneuver (left lateral decubitus with head-down positioning) to optimize right ventricular outflow dynamics. Most patients achieve complete resolution within 36 to 48 hours using these conservative measures. Advanced therapies such as hyperbaric oxygen or surgical air extraction are typically reserved for hemodynamically unstable patients or those showing signs of end-organ compromise [2,3].
This case demonstrates an acute clinical deterioration due to massive air embolism with progressive multi-organ failure that proved refractory to all therapeutic interventions, ultimately resulting in an irreversible clinical course despite maximal supportive care.

Figure 1: Presence of air in the lumen of the right ventricle.
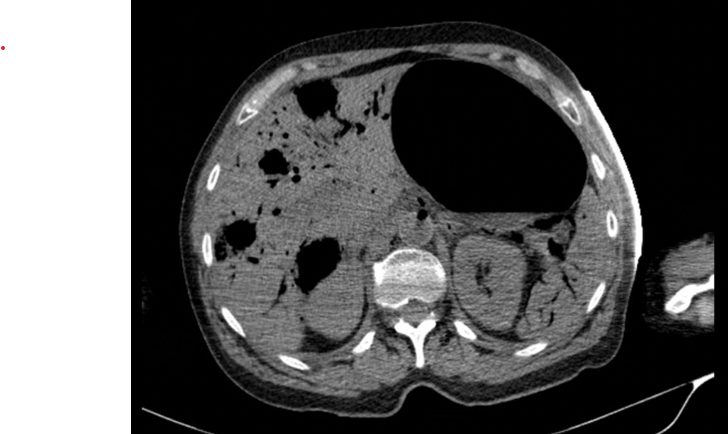
Figure 2: Air in the lumen of multiple vascular structures.
The figure 2 shows the presence of air in the lumen of the middle and left hepatic veins, with gaseous content in multiple vascular structures with a branched appearance in both lobes of the liver and gaseous structures/collections with multiple millimetric air bubbles in the liver parenchyma that communicate with the vascular structures; we can also see air in the vessels of the splenic hilum and intrasplenic vascular structures.